Vol 6 No 1 2021 – 25
REPORTE DE CASOS / CASE REPORTS
Fungoide Mycosis. Case report
Irene Rojas Rondón1, Lázaro Vigoa Aranguren1, Maritza Miqueli Rodríguez1, María de Lourdes Guzmán Martínez1, Manuel Alejandro Múzquiz Jiménez1
Available from: http://dx.doi.org/10.21931/RB/2021.06.01.25
ABSTRACT
To report the case of a 63-years-old female referred to the Oculoplastic Eyelid and Orbit Department of the ICO «Ramón Pando Ferrer» for two lesions in the left upper eyelid, the biggest one, a 20 mm nodule with a central ulcer full of debris and discharge. It was treated with antibiotics without improvement; a biopsy was carried out with a preliminary report of Mycosis Fungoides. A similar lesion appeared on the lower eyelid after surgery and was treated with perilesional HeberFERON injections, disappearing after three weeks. The final histopathology analysis revealed a Non-Hodgkin skin lymphoma with a high malignancy grade. Conclusions: Diagnosing Mycosis fungoides is difficult in early stages or atypical presentations. It’s essential to know this disease and its stages to set it apart from entities with similar characteristics, aiming for an early diagnosis, treatment, and proper follow-up.
Keywords: Mycosis fungoides. Cutaneous lymphoma. HeberFERON. Eyelid tumors. Interferons.
INTRODUCTION
The first description of Mycosis fungoides (MF) is documented in Alibert’s Dermatology Atlas (1768-1837); he described in France the case of a 56-year-old man who presented skin desquamation followed by the apparition of several tumors disseminated on the body, which aspect and consistency reminded the mushrooms, therefore the name. The term is quite ambiguous, and it vaguely means «disease that looks like a fungus» 1, 2.
In 1870, Pierre Antoine Ernest Bazin made a more detailed description of the clinical phases: eczematous, plaque, and tumoral. After that, in the late XIX century, they discovered that the tumors could appear skipping the prior stages, giving this variety the name «micosis fungoidee demblée» or «primitive mycosis fungoide»1, 2.
Some authors refer that this disease shows a preference for males (1.6-2:1) and is more common in middle-aged adults (50 years), although it has been documented in adolescents. It has a higher incidence in highly pigmented races1-6.
Nevertheless, the most frequent Lymphoma type (44%), the Non-Hodgkin Extranodal Mature T-Cell Lymphoma that affects the skin, is still a rare condition 3, 9.
The diagnosis for T-Cell Cutaneous Lymphoma (TCCL) is based on the histopathological and clinical evidence; the immunohistochemistry ascertains the immune-phenotype based on the surface markers lymphocytic infiltrates. The markers used show the predominance of B-Cells or T-Cells and the presence of Natural Killer Lymphocites1,2, 5, 7.
The tumors can appear over the preexisting plaques, showing vertical growth. When the lesions appear, the Novo suggests malign T-Cell invasion. At this stage, the entity shows a predilection for the face and skin folds. The presence of nodules and tumors is frequent, and they tend to ulcer and get infected 1, 3, 9.
Ancillary tests include full blood count, peripheral blood smear, a skin biopsy (may need more than one), immune- phenotypification, T-Cell receptor gene rearrangement test, flow cytometry, chest X-ray, CT Scan, PET Scan, and bone marrow biopsy to stage the disease 1-3, 9.
There are different treatment options. The five standard procedures are: photodynamic therapy, radiotherapy, chemotherapy, pharmacologic therapy, and biologic agents, and new treatment options are under investigation.1, 5, 8, 9
Case
A 63-years-old female was referred to the Oculoplastic Department in our hospital, with the chief complaint of two lesions in the left upper eyelid. The lesions appeared 15 days before the consultation and were treated with an oral antibiotic (ciprofloxacin 500mg twice/day for 7 days). The patient suffered viral conjunctivitis two weeks before the tumor’s apparition, and it disappeared with hygienic measures.
The patient had two tumors in the left upper eyelid, close to the other, one of them at the nasal area, measured 20mm approximately, nodular with a central ulcer full of debris and discharge; the second tumor was erythematous, about 3-4mm (figure 1). There were not growing regional lymph nodes, and it also appeared to concurrent with an infectious process, so the antibiotic treatment was extended, adding chloramphenicol ointment three times/day for 15 days. The lesions were getting worse at the end of this treatment.

Figure 1. 63-year-old female with two lesions on the left upper eyelid, the biggest one measured 20mm, was nodular with a central ulcer full of debris, the other lesion was near, resembled an erythematous plaque and measuring 3mm.
The quick tumoral growth caused ptosis of the left eyelid (figure 2). We planned the excision of the masses and palpebral reconstruction under local anesthesia. The procedure had good functional and esthetic outcomes.

Figure 2. The tumoral growth caused eyelid ptosis. This image shows the smaller lesion, an erythematous 3mm plaque.
After the excision, before the histopathological analysis, a new lesion appeared on the lower left eyelid with similar characteristics and evolution to the upper eyelid ones; and also existed erythematous lesions at the right forearm (figure 3).


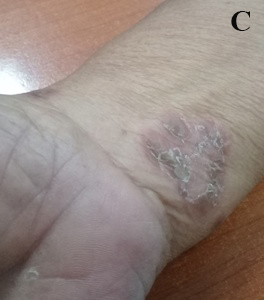
Figure 3. A: Lower left eyelid tumor, was about 1cm, nodular, a central ulcer, and eyelid erythema. B and C: On the right forearm and upper arm existed erythematous plaques.
The histopathological analysis was compatible with Mycosis fungoides, but the pathologist wanted a second opinion. We decided to infiltrate HeberFERON on the surrounding area with this possible diagnosis while waiting for confirmation of biopsy because this treatment would be useful for both possible entities. The treatment was 3.5UI twice a week, for five weeks. The tumor reduced its size after the second dose and disappeared after the third week (figure 4). The arm lesions also disappeared.
The final biopsy determined it was a Non-Hodgkin diffuse skin lymphoma, with a high malignancy grade.


Figure 4. A: Lower eyelid lesion reduced its size after the second dose. B: The tumor disappeared in the third week after the use of HeberFERON. The patient was referred to a dermatology specialist after the diagnosis was confirmed.
DISCUSSION
The first likely diagnosis was an infection of the eyelid skin, supported by the lesion’s characteristics (full of debris, yellow discharge, and erythema), the smaller tumor, the intense itching, and viral conjunctivitis that resolved spontaneously. The possibility of a malign tumor of the eyelid accompanied by sepsis wasn’t ruled out, as the sepsis can mask the tumor characteristics, adding difficulties to the diagnostic process. The literature also mentions multiple keratoacanthomata, very infrequent 10, anyways, we decided to treat the infectious process and re-evaluate the tumor to decide the next step.
Because of the rapid growth and eyelid ptosis, we decided to remove the tumor. The histopathological diagnosis was skin infection vs. keratoacanthoma. The excision with oncological margins caused a severe defect on the eyelid and necessary reconstruction with a rotated skin graft. While we waited for the definitive biopsy result, a new tumor appeared on the lower eyelid, with a similar appearance and growth.
The new lesion’s apparition made us keep the differential diagnosis of a viral infection, as it didn’t respond to the antibiotics. It is known that keratoacanthoma can have a viral etiology and appear in multiple lesions, although this is controversial10. The presence of multiple malign tumors made us think about syndromic causes, although it’s relatively infrequent in aged patients, and they don’t resemble basal carcinomas, so we discarded this diagnostic possibility.
The anatomopathological diagnostic impression was an MF, and the pathologist required a second specialist opinion, with more experience in this kind of disease, as it is an uncommon entity. With this differential diagnosis and the possibility of a viral infection, we decided to wait for the biopsy confirmation. Instead of performing surgical excision of the lower eyelid lesion, we started to infiltrate the surrounding tissue with HeberFERON, as it is used in both entities 1-3, 10. The treatment was 3.5UI twice/week for five weeks. The tumor reduced its size after the second dose and disappeared after the third week.
The final biopsy reported a Non-Hodgkin diffuse skin lymphoma clinically on the tumoral phase, with a high malignancy grade. We decided to refer the patient to another Institute with Dermatological Department.
Every patient with MF diagnosis, likely or confirmed, must be referred as soon as possible to a dermatologist to confirm the diagnosis and start to treat it accordingly to its phase.
The dermatological affections with eyelid lesions form part of a great group of diseases. For its location and way of the apparition, the patients look for an ophthalmologist instead of a dermatologist. Its similitude with other entities as eyelid infections, malign eyelid tumors, keratoacanthoma, basal cell carcinoma, atypical psoriasis, and others can delay diagnosis treatment.
The histopathological typification as an MF is difficult at the early phases, as the typical characteristics may be absent. Sometimes more than one biopsy is needed to confirm the diagnosis and the differential diagnosis with another kind of lymphoma has to be made 1, 3, 6,7.
Biological therapy is a treatment to stimulate the patient’s immune system to combat the tumor. It uses substances produced by the body or at the lab to urge a response or restore cancer’s physiological reactions. The Interferon is used to treat multiple entities: viral infections, MF, and other tumors. It alters the cell division, slowing down the tumor’s growth, giving time to the immune system to eliminate it 1, 3, 7, 10; therefore, we decided to inject HeberFERON on the surrounding tissue, getting great results.
The prognosis of MF is variable and depends on the stage in which the diagnosis was made, the subtype, extension, and the presence of extracutaneous affection. Nowadays, several atypical subtypes have been documented, each very different from the classic forms, giving the disease the title of «great simulator,» the reason why one must keep it in mind as a diagnostic possibility 1, 3, 6-7.
MF has a difficult diagnosis in early stages or unusual presentations and must be a differential diagnosis for eyelid lesions with atypical characteristics. The correlation of clinic and anatomopathological characteristics is the keystone to making an early diagnosis 1-3, 5, 9.
CONCLUSION
It is essential to know this entity and its different stages to differentiate it from other diagnosis with similar lesions to avoid delay of the diagnosis and treatment in patients with Mycosis fungoides.
REFERENCES
1. Calzado Villarreal L. Linfomas cutáneos de células T (Micosis fungoide / síndrome Sezary): estudio de factores predictivos de progresión y de remisión completa a primer tratamiento. [TESIS]. Universidad Complutense de Madrid. Facultad de Medicina; 2016.
2. González Ramírez RA, Ocampo Candiani J, Méndez Olvera N, Gómez Flores M. Micosis fungoide: Biología y terapéutica Dermatología CMQ. 2006;4(4):278-287.
3. Junco Bonet M, Betancourt Betancourt G, Machado García GJ, Larquin Comet JI. Micosis fungoide en estadio tumoral: Presentación de un caso. Rev. Arch Med Camagüey. 2016;20(1):44-49.
4. Gül U, Soylu S, Aslan E, Yazar Z, Demíríz M. Uncommon presentation of mycosis fungoides: Eyelid margin involvement. J Dermatol. 2008;35(9):581-4.
5. Wieser I, Huean A, Bush AE, Dabaja BS, Duvic M. Periorbital Involvement in Early Stage Mycosis Fungoides. Acta Derm Venereol. 2017; 97(8):976-8.
6. Jesufbegovic D, Char DH. Clinical Variability of Ocular Involvement in Mycosis Fungoides. JAMA Ophthalmol. 2015;133(3):341-3.
7. Martínez Piva MM, Zambrano Franco EA, Kowalczuk AM, Enz PA. Variantes atípicas de micosis fungoide: estudio de cohorte retrospectivo de 15 años. Med Cutan Iber Lat Am. 2017;45(3):185-190.
8. Goggins CA, Gocke MT, Jang S, DeSimone JA. Oral Mycosis fungoide with CD30+ large cell transformation successfully treated with brentuximab vedotin. JAAD Case Rep. 2019;5(2):180-3.
9. Hwa Lim E, Ki Lim S, Im M, Joon Seo Y, Hoon Lee Y, Lee Y. Mycosis Fungoides Diagnosis with an Initial Sign Resembling Benign Dermatosis on the Upper Eyelids. Ann Dermatol. 2015; 27(4):469-71.
10. Rojas Rondón I, Agramonte Centelles IC, Río Torres M. Afecciones palpebrales. La Habana: Editorial Ciencias Médicas; 2018.
Received:24 November 2020
Accepted: 15 January 2021
Irene Rojas Rondón1, Lázaro Vigoa Aranguren1, Maritza Miqueli Rodríguez1, María de Lourdes Guzmán Martínez1, Manuel Alejandro Múzquiz Jiménez1
1. Instituto Cubano de Oftalmología “Ramón Pando Ferrer”. La Habana, Cuba.
Autor de correspondencia: Dra. Irene Rojas Rondón
Jefa del departamento de Cirugía Plástica Ocular
Corresponding author: irojas@infomed.sld.cu
Dirección Postal: 11500
Dirección: Calle 76 #3104 % 31 y 41. Municipio Marianao. Ciudad de la Habana. Cuba.



















